18 results
Association between job role and coronavirus disease 2019 (COVID-19) among healthcare personnel, Iowa, 2021
- Takaaki Kobayashi, Alexandra Trannel, John Heinemann, Alexandre R. Marra, William Etienne, Oluchi J. Abosi, Stephanie Holley, Angelique Dains, Kyle E. Jenn, Holly Meacham, Barbara A. Schuessler, Linder Wendt, Patrick Ten Eyck, Beth Hanna, Jorge L. Salinas, Patrick G. Hartley, Bradley Ford, Melanie Wellington, Karen B. Brust, Daniel J. Diekema
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 01 December 2022, e188
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We describe the association between job roles and coronavirus disease 2019 (COVID-19) among healthcare personnel. A wide range of hazard ratios were observed across job roles. Medical assistants had higher hazard ratios than nurses, while attending physicians, food service workers, laboratory technicians, pharmacists, residents and fellows, and temporary workers had lower hazard ratios.
Coronavirus disease 2019 (COVID-19) among nonphysician healthcare personnel by work location at a tertiary-care center, Iowa, 2020–2021
- Part of
- Takaaki Kobayashi, John Heinemann, Alexandra Trannel, Alexandre R. Marra, Mohammed Alsuhaibani, William Etienne, Lorinda L. Sheeler, Oluchi Abosi, Stephanie Holley, Mary Beth Kukla, Angelique Dains, Kyle E. Jenn, Holly Meacham, Beth Hanna, Bradley Ford, Karen Brust, Melanie Wellington, Patrick G. Hartley, Daniel J. Diekema, Jorge L. Salinas
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 8 / August 2023
- Published online by Cambridge University Press:
- 02 June 2022, pp. 1351-1354
- Print publication:
- August 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We describe COVID-19 cases among nonphysician healthcare personnel (HCP) by work location. The proportion of HCP with coronavirus disease 2019 (COVID-19) was highest in the emergency department and lowest among those working remotely. COVID-19 and non–COVID-19 units had similar proportions of HCP with COVID-19 (13%). Cases decreased across all work locations following COVID-19 vaccination.
COVID-19 incidence among nonphysician healthcare workers at a tertiary care center–Iowa, 2020–2021
- Takaaki Kobayashi, John Heinemann, Alexandra Trannel, Alexandre Marra, William Etienne, Oluchi Abosi, Stephanie Holley, Mary Kukla, Angie Dains, Kyle Jenn, Holly Meacham, Beth Hanna, Bradley Ford, Melanie Wellington, Patrick Hartley, Daniel Diekema, Jorge Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s6-s7
-
- Article
-
- You have access Access
- Open access
- Export citation
-
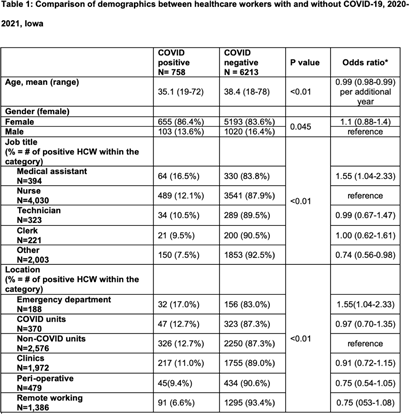
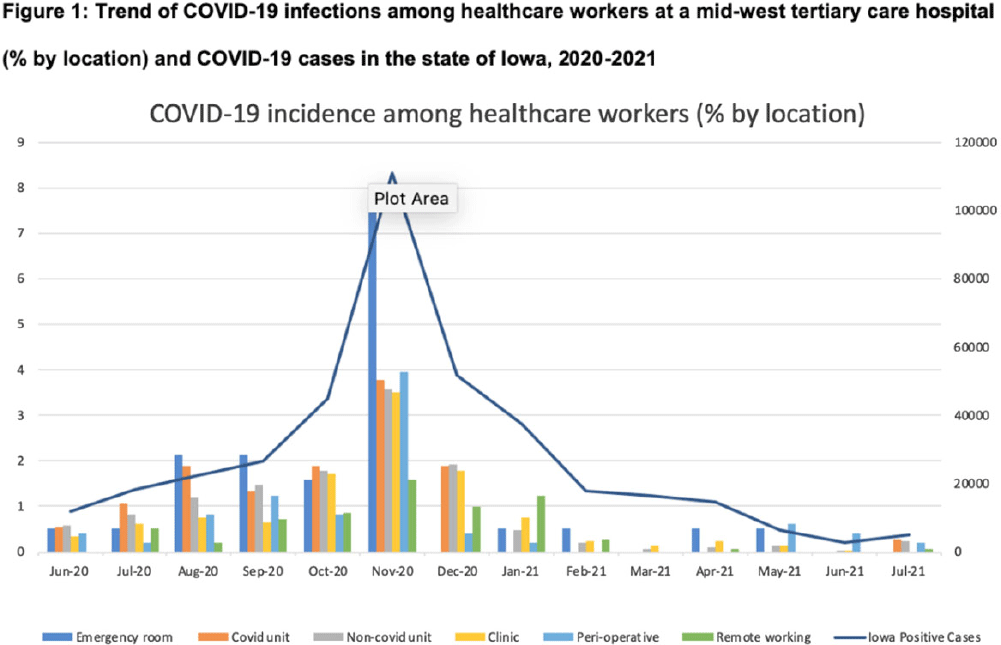
Background: Whether working on COVID-19 designated units put healthcare workers (HCWs) at higher risk of acquiring COVID-19 is not fully understood. We report trends of COVID-19 incidence among nonphysician HCWs and the association between the risk of acquiring COVID-19 and work location in the hospital. Methods: The University of Iowa Hospitals & Clinics (UIHC) is an 811-bed, academic medical center serving as a referral center for Iowa. We retrospectively collected COVID-19–associated data for nonphysician HCWs from Employee Health Clinic between June 1st 2020 and July 31th 2021. The data we abstracted included age, sex, job title, working location, history of COVID-19, and date of positive COVID-19 test if they had a history of COVID-19. We excluded HCWs who did not have a designated working location and those who worked on multiple units during the same shift (eg, medicine resident, hospitalist, etc) to assess the association between COVID-19 infections and working location. Job titles were divided into the following 5 categories: (1) nurse, (2) medical assistant (MA), (3) technician, (4) clerk, and (5) others (eg patient access, billing office, etc). Working locations were divided into the following 6 categories: (1) emergency department (ED), (2) COVID-19 unit, (3) non–COVID-19 unit, (4) Clinic, (5) perioperative units, and (6) remote work. Results: We identified 6,971 HCWs with work locations recorded. During the study period, 758 HCWs (10.8%) reported being diagnosed with COVID-19. Of these 758 COVID-19 cases, 658 (86.8%) were diagnosed before vaccines became available. The location with the highest COVID-19 incidence was the ED (17%), followed by both COVID-19 and non–COVID-19 units (12.7%), clinics (11.0%), perioperative units (9.4%) and remote work stations (6.6%, p Conclusions: Strict and special infection control strategies may be needed for HCWs in the ED, especially where vaccine uptake is low. The administrative control of HCWs working remotely may be associated with a lower incidence of COVID-19. Given that the difference in COVID-19 incidence among HCWs by location was lower and comparable after the availability of COVID-19 vaccines, facilities should make COVID-19 vaccination mandatory as a condition of employment for all HCWs, especially in areas where the COVID-19 incidence is high.
Funding: None
Disclosures: None
Blood-culture ordering practices in patients with a central line at an academic medical center–Iowa, 2020
- Elias Kovoor, Takaaki Kobayashi, Lorinda Sheeler, Alexandra Trannel, William Etienne, Oluchi Abosi, Stephanie Holley, Mary Kukla, Angie Dains, Kyle Jenn, Holly Meacham, Beth Hanna, Alexandre Marra, Meredith Parsons, Bradley Ford, Melanie Wellington, Daniel Diekema, Jorge Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, p. s30
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The IDSA has a clinical definition for catheter-related bloodstream infection (CRBSI) that requires ≥1 set of blood cultures from the catheter and ≥1 set from a peripheral vein. However, because blood cultures obtained from a central line may represent contamination rather than true infection, many institutions discourage blood cultures from central lines. We describe blood culture ordering practices in patients with a central line. Methods: The University of Iowa Hospitals & Clinics is an academic medical center with 860 hospital beds. We retrospectively collected data for blood cultures obtained from adult patients (aged ≥18 years) in the emergency department or an inpatient unit during 2020. We focused on the first blood cultures obtained during each admission because they are usually obtained before antibiotic initiation and are the most important opportunity to diagnose bacteremia. We classified blood-culture orders as follows: CRBSI workup, non-CRBSI sepsis workup, or incomplete workup. We defined CRBSI workup as ≥1 blood culture from a central line and ≥1 peripheral blood culture (IDSA guidelines). We defined non-CRBSI sepsis workup as ≥2 peripheral blood cultures without cultures from a central line because providers might have suspected secondary bacteremia rather than CRBSI. We defined incomplete workup as any order that did not meet the CRBSI or non-CRBSI sepsis workup. This occurred when only 1 peripheral culture was obtained or when ≥1 central-line culture was obtained without peripheral cultures. Results: We included 1,150 patient admissions with 4,071 blood cultures. In total, 349 patient admissions with blood culture orders (30.4%) met CRBSI workup. 62.8% were deemed non-CRBSI sepsis workup, and 6.9% were deemed an incomplete workup. Stratified by location, ICUs had the highest percentage of orders with incomplete workups (8.8%), followed by wards (7.2%) and the emergency department (5.1%). In total, 204 patient admissions had ≥1 positive blood culture (17.7%). The most frequently isolated organisms were Staphylococcus epidermidis (n = 33, 16.2%), Staphylococcus aureus (n = 16, 7.8%), and Escherichia coli (n = 15, 7.4%) Conclusions: Analysis of blood culture data allowed us to identify units at our institute that were underperforming in terms of ordering the necessary blood cultures to diagnose CRBSI. Being familiar with CRBSI guidelines as well as decreasing inappropriate ordering will help lead to early and proper diagnosis of CRBSI which can reduce its morbidity, mortality, and cost.
Funding: None
Disclosures: None
Blood culture practices in patients with a central line at an academic medical center—Iowa, 2020
- Elias Kovoor, Takaaki Kobayashi, Lorinda L. Sheeler, Alexandra Trannel, William Etienne, Oluchi Abosi, Stephanie Holley, Angelique Dains, Kyle E. Jenn, Holly Meacham, Beth Hanna, Alexandre R. Marra, Meredith Parsons, Bradley Ford, Melanie Wellington, Daniel J. Diekema, Jorge L. Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 13 April 2022, e64
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We analyzed blood-culture practices to characterize the utilization of the Infectious Diseases Society of America (IDSA) recommendations related to catheter-related bloodstream infection (CRBSI) blood cultures. Most patients with a central line had only peripheral blood cultures. Increasing the utilization of CRBSI guidelines may improve clinical care, but may also affect other quality metrics.
Molecular Epidemiology of Large COVID-19 Clusters at an Academic Medical Center, March–October 2020
- Takaaki Kobayashi, Miguel Ortiz, Stephanie Holley, William Etienne, Kyle Jenn, Oluchi Abosi, Holly Meacham, Lorinda Sheeler, Angie Dains, Mary Kukla, Alexandra Trannel, Alexandre Marra, Mohammed Alsuhaibani, Paul McCray, Stanley Perlman, Bradley Ford, Daniel Diekema, Melanie Wellington, Alejandro Pezzulo, Jorge Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s10-s11
-
- Article
-
- You have access Access
- Open access
- Export citation
-
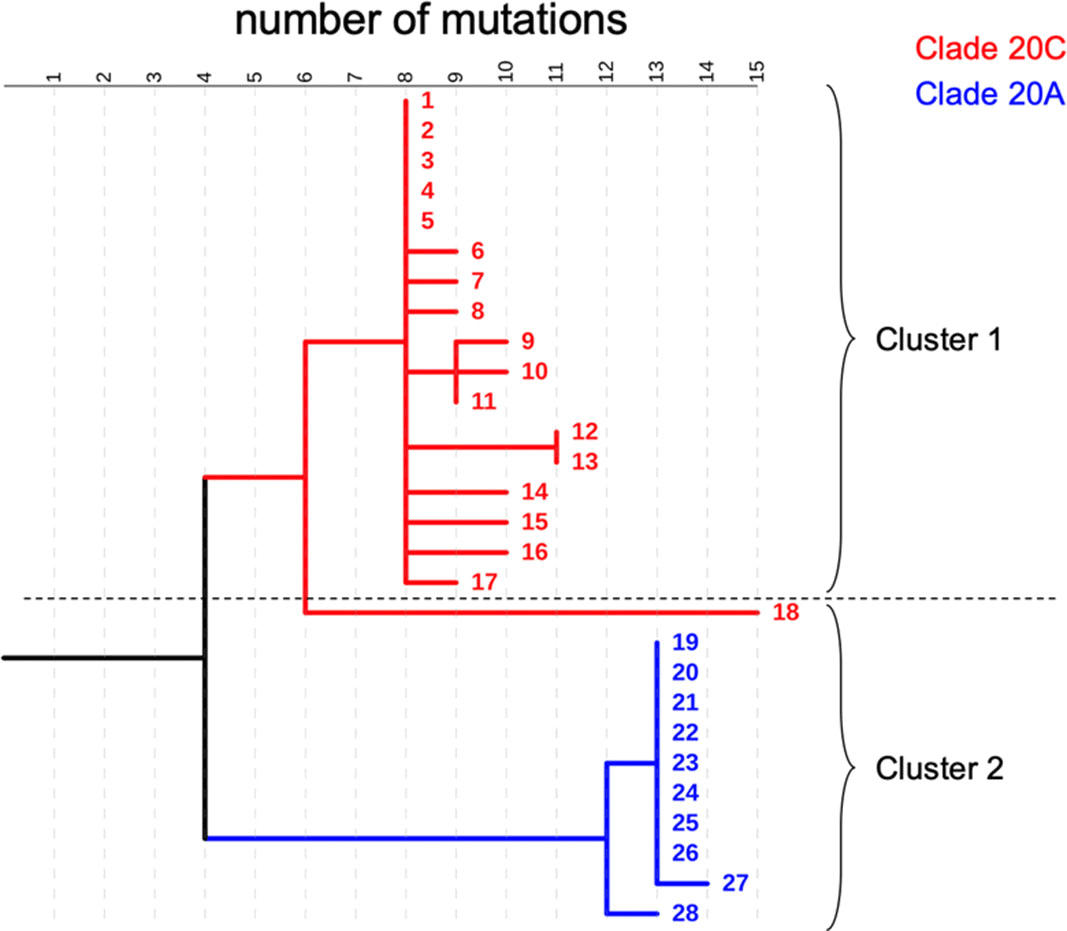
Background: COVID-19 in hospitalized patients may be the result of community acquisition or in-hospital transmission. Molecular epidemiology can help confirm hospital COVID-19 transmission and outbreaks. We describe large COVID-19 clusters identified in our hospital and apply molecular epidemiology to confirm outbreaks. Methods: The University of Iowa Hospitals and Clinics is an 811-bed academic medical center. We identified large clusters involving patients with hospital onset COVID-19 detected during March–October 2020. Large clusters included ≥10 individuals (patients, visitors, or HCWs) with a laboratory confirmed COVID-19 diagnosis (RT-PCR) and an epidemiologic link. Epidemiologic links were defined as hospitalization, work, or visiting in the same unit during the incubation or infectious period for the index case. Hospital onset was defined as a COVID-19 diagnosis ≥14 days from admission date. Admission screening has been conducted since May 2020 and serial testing (every 5 days) since July 2020. Nasopharyngeal swab specimens were retrieved for viral whole-genome sequencing (WGS). Cluster patients with a pairwise difference in ≤5 mutations were considered part of an outbreak. WGS was performed using Oxford Nanopore Technology and protocols from the ARTIC network. Results: We identified 2 large clusters involving patients with hospital-onset COVID-19. Cluster 1: 2 hospital-onset cases were identified in a medical-surgical unit in June 2020. Source and contact tracing revealed 4 additional patients, 1 visitor, and 13 employees with COVID-19. Median age for patients was 62 (range, 38–79), and all were male. In total, 17 samples (6 patients, 1 visitor, and 10 HCWs) were available for WGS. Cluster 2: A hospital-onset case was identified via serial testing in a non–COVID-19 intensive care unit in September 2020. Source investigation, contact tracing, and serial testing revealed 3 additional patients, and 8 HCWs. One HCW also had a community exposure. Patient median age was 60 years (range, 48–68) and all were male. In total, 11 samples (4 patients and 7 HCWs) were sequenced. Using WGS, cluster 1 was confirmed to be an outbreak: WGS showed 0–5 mutations in between samples. Cluster 2 was also an outbreak: WGS showed less diversity (0–3 mutations) and ruled out the HCW with a community exposure (20 mutations of difference). Conclusion: Whole-genome sequencing confirmed the outbreaks identified using classic epidemiologic methods. Serial testing allowed for early outbreak detection. Early outbreak detection and implementation of control measures may decrease outbreak size and genetic diversity.
Funding: No
Disclosures: None
Figure 1.
COVID-19 Conversion after Exposure in a Semiprivate Room at a Tertiary Care Center in Iowa, July–December 2020
- Alexandra Trannel, Takaaki Kobayashi, Oluchi Abosi, Kyle Jenn, Holly Meacham, Lorinda Sheeler, William Etienne, Angie Dains, Mary Kukla, Mohammed Alsuhaibani, Stephanie Holley, Alexandre Marra, Bradley Ford, Melanie Wellington, Daniel Diekema, Jorge Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, pp. s20-s21
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Hospital semiprivate rooms may lead to coronavirus disease 2019 (COVID-19) patient exposures. We investigated the risk of COVID-19 patient-to-patient exposure in semiprivate rooms and the subsequent risk of acquiring COVID-19. Methods: The University of Iowa Hospitals & Clinics is an 811-bed tertiary care center. Overall, 16% of patient days are spent in semiprivate rooms. Most patients do not wear masks while in semiprivate rooms. Active COVID-19 surveillance included admission and every 5 days nasopharyngeal SARS-CoV-2 polymerase chain reaction (PCR) testing. We identified inpatients with COVID-19 who were in semiprivate rooms during their infectious periods during July–December 2020. Testing was repeated 24 hours after the first positive test. Cycle threshold (Ct) values of the two tests (average Ct <30), SARS-CoV-2 serology results, clinical assessment, and COVID-19 history were used to determine patient infectiousness. Roommates were considered exposed if in the same semiprivate room with an infectious patient. Exposed patients were notified, quarantined (private room), and follow-up testing was arranged (median seven days). Conversion was defined as having a negative test followed by a subsequent positive within 14 days after exposure. We calculated the risk of exposure: number of infectious patients in semiprivate rooms/number of semiprivate patient-days (hospitalization days in semiprivate rooms). Results: There were 16,427 semiprivate patient days during July–December 2020. We identified 43 COVID-19 inpatients who roommates during their infectious periods. Most infectious patients (77%) were male; the median age was 67 years; and 22 (51%) were symptomatic. Most were detected during active surveillance: admission testing (51%) and serial testing (28%). There were 57 exposed roommates. The risk of exposure was 3 of 1,000 semiprivate patient days. In total, 16 roommates (28%) did not complete follow-up testing. Of 41 exposed patients with follow-up data, 8 (20%) converted following their exposure. Median time to conversion was 5 days. The risk of exposure and subsequent conversion was 0.7 of 1,000 semiprivate patient days. Median Ct value of the source patient was 20 for those who converted and 23 for those who did not convert. Median exposure time was 45 hours (range, 3–73) for those who converted and 12 hours (range, 1–75) for those who did not convert. Conclusions: The overall risk of exposure in semiprivate rooms was low. The conversion rate was comparable to that reported for household exposures. Lower Ct values and lengthier exposures may be associated with conversion. Active COVID-19 surveillance helps early detection and decreases exposure time.
Funding: No
Disclosures: None
Coronavirus Disease 2019 (COVID-19) Admission Screening at a Tertiary-Care Center, Iowa 2020
- Mohammed Alsuhaibani, Takaaki Kobayashi, Alexandra Trannel, Stephanie Holley, Oluchi Abosi, Kyle Jenn, Holly Meacham, Lorinda Sheeler, William Etienne, Angie Dains, Mary Kukla, Emily Ward, Bradley Ford, Michael Edmond, Melanie Wellington, Daniel Diekema, Jorge Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Hospitalized patients may unknowingly carry severe acute respiratory coronavirus virus 2 (SARS-CoV-2), even if they are admitted for other reasons. Because SARS-CoV-2 may remain positive by reverse-transcriptase polymerase chain reaction (RT-PCR) for months after infection, patients with a positive result may not necessarily be infectious. We aimed to determine the frequency of SARS-CoV-2 infections in patients admitted for reasons unrelated to coronavirus disease 2019 (COVID-19). Methods: The University of Iowa Hospitals and Clinics is an 811-bed tertiary-care center. We use a nasopharyngeal SARS-CoV-2 RT-PCR to screen admitted patients without signs or symptoms compatible with COVID-19. Patients with positive tests undergo a repeat test to assess cycle threshold (Ct) value kinetics. We reviewed records for patients with positive RT-PCR screening admitted during July–October 2020. We used a combination of history, serologies, and RT-PCR Ct values to assess and qualify likelihood of infectiousness: (1) likely infectious, if Ct values were <29, or (2) likely not infectious, if 1 or both samples had Cts <30 with or without a positive SARS-CoV-2 antinucleocapsid IgG/IgM test or history of a positive result in the past 90 days. Contact tracing was only conducted for patients likely to be infectious. We describe the isolation duration and contact tracing data. Results: In total, 6,447 patients were tested on hospital admission for any reason (persons under investigation or admitted for reasons other than COVID-19). Of these, 240 (4%) had positive results, but 65 (27%) of these were admitted for reasons other than COVID-19. In total, 55 patients had Ct values available and were included in this analysis. The median age was 56 years (range, 0–91), 28 (51%) were male, and 12 (5%) were children. The most frequent admission syndromes were neurological (36%), gastrointestinal (16%), and trauma (16%). Our assessment revealed 23 likely infections (42%; 14 definite, 9 possible) and 32 cases likely not infectious (58%). The mean Ct for patients who were likely infectious was 22; it was 34 for patients who were likely not infectious. Mean duration of in-hospital isolation was 6 days for those who were likely infectious and 2 days for those who were likely not infectious. We detected 8 individuals (1 healthcare worker and 7 patients) who were exposed to a likely infectious patient. Conclusions: SARS-CoV-2 infection in patients hospitalized for other reasons was infrequent. An assessment of the likelihood of infectiousness including history, RT-PCR Cts, and serology may help prioritize patients in need of isolation and contact investigations.
Funding: No
Disclosures: None
Suspected COVID-19 Reinfections at a Tertiary Care Center, Iowa 2020
- Takaaki Kobayashi, Mohammed Alsuhaibani, Miguel Ortiz, Katherine Imborek, Stephanie Holley, Alexandra Trannel, Alexandre Marra, William Etienne, Kyle Jenn, Oluchi Abosi, Holly Meacham, Lorinda Sheeler, Angie Dains, Mary Kukla, Paul McCray, Stanley Perlman, Bradley Ford, Daniel Diekema, Melanie Wellington, Alejandro Pezzulo, Jorge Salinas
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s19
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Coronavirus disease 2019 (COVID-19) is caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). SARS-CoV-2 RNA can be detected by real-time reverse-transcription polymerase chain reaction (RT-PCR) for several weeks after infection. Discerning persistent RT-PCR positivity versus reinfection is challenging and the frequency of COVID-19 reinfections is unknown. We aimed to determine the frequency of clinically suspected reinfection in our center and confirm reinfection using viral whole-genome sequencing (WGS). Methods: The University of Iowa Hospitals and Clinics (UIHC) is an 811-bed academic medical center. Patients with respiratory complaints undergo COVID-19 RT-PCR using nasopharyngeal swabs. The RT-PCR (TaqPath COVID-19 Combo kit) uses 3 targets (ORF1ab, S gene, and N gene). We identified patients with previous laboratory-confirmed COVID-19 who sought care for new respiratory complaints and underwent a repeated SARS-CoV-2 test at least 45 days from their first positive test. We then identified patients with median RT-PCR cycle threshold (Ct) values. Results: During the study period, 13,603 patients had a SARS-CoV-2– positive RT-PCR. Of these, 296 (2.2%) had a clinical visit for new onset of symptoms and a repeated RT-PCR assay >45 days from the first test. Moreover, 29 patients (9.8%) had a positive RT-PCR assay in the repeated testing. Ct values were available for samples from 25 patients; 7 (28%) had Ct values. Conclusions: In patients with a recent history of COVID-19 infection, repeated testing for respiratory symptoms was infrequent. Some had a SARS-CoV-2–positive RT-PCR assay on repeated testing, but only 1 in 4 had Ct values suggestive of a reinfection. We confirmed 1 case of reinfection using WGS.
Funding: No
Disclosures: None
Coronavirus disease 2019 (COVID-19) incidence after exposures in shared patient rooms in a tertiary-care center in Iowa, July 2020–May 2021
- Part of
- Alexandra M. Trannel, Takaaki Kobayashi, Angelique Dains, Oluchi J. Abosi, Kyle E. Jenn, Holly Meacham, Lorinda L. Sheeler, William Etienne, Mary E. Kukla, Mohammed Alsuhaibani, Stephanie Holley, Kelsey Strandberg, Alexandre R. Marra, Jeffrey Kritzman, Bradley Ford, Melanie Wellington, Daniel J. Diekema, Jorge L. Salinas
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 12 / December 2022
- Published online by Cambridge University Press:
- 12 July 2021, pp. 1910-1913
- Print publication:
- December 2022
-
- Article
- Export citation
-
The incidence of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) exposure in shared patient rooms was low at our institution: 1.8 per 1,000 shared-room patient days. However, the secondary attack rate (21.6%) was comparable to that reported in household exposures. Lengthier exposures were associated with SARS-CoV-2 conversion. Hospitals should implement measures to decrease shared-room exposures.
Coronavirus disease 2019 (COVID-19) admission screening and assessment of infectiousness at an academic medical center in Iowa, 2020
- Part of
- Mohammed A. Alsuhaibani, Takaaki Kobayashi, Alexandra Trannel, Stephanie Holley, Oluchi J. Abosi, Kyle E. Jenn, Holly Meacham, Lorinda Sheeler, William Etienne, Angelique Dains, Mary E. Kukla, Emily Ward, Bradley Ford, Michael B. Edmond, Melanie Wellington, Daniel J. Diekema, Jorge L. Salinas
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 43 / Issue 8 / August 2022
- Published online by Cambridge University Press:
- 24 June 2021, pp. 974-978
- Print publication:
- August 2022
-
- Article
- Export citation
-
Objective:
Patients admitted to the hospital may unknowingly carry severe acute respiratory coronavirus virus 2 (SARS-CoV-2), and hospitals have implemented SARS-CoV-2 admission screening. However, because SARS-CoV-2 reverse-transcription polymerase chain reaction (RT-PCR) assays may remain positive for months after infection, positive results may represent active or past infection. We determined the prevalence and infectiousness of patients who were admitted for reasons unrelated to COVID-19 but tested positive for SARS-CoV-2 on admission screening.
Methods:We conducted an observational study at the University of Iowa Hospitals & Clinics from July 7 to October 25, 2020. All patients admitted without suspicion of COVID-19 were included, and medical records of those with a positive admission screening test were reviewed. Infectiousness was determined using patient history, PCR cycle threshold (Ct) value, and serology.
Results:In total, 5,913 patients were screened and admitted for reasons unrelated to COVID-19. Of these, 101 had positive admission RT-PCR results; 36 of these patients were excluded because they had respiratory signs/symptoms on admission on chart review. Also, 65 patients (1.1%) did not have respiratory symptoms. Finally, 55 patients had Ct values available and were included in this analysis. The median age of the final cohort was 56 years and 51% were male. Our assessment revealed that 23 patients (42%) were likely infectious. The median duration of in-hospital isolation was 5 days for those likely infectious and 2 days for those deemed noninfectious.
Conclusions:SARS-CoV-2 was infrequent among patients admitted for reasons unrelated to COVID-19. An assessment of the likelihood of infectiousness using clinical history, RT-PCR Ct values, and serology may help in making the determination to discontinue isolation and conserve resources.
Molecular epidemiology of large coronavirus disease 2019 (COVID-19) clusters before and after the implementation of routine serial testing at an academic medical center in Iowa, 2020
- Part of
- Miguel E. Ortiz, Takaaki Kobayashi, Katherine Imborek, Mohammed Alsuhaibani, Stephanie Holley, Alexandra Trannel, Alexandre R. Marra, William Etienne, Kyle E. Jenn, Oluchi J. Abosi, Holly Meacham, Lorinda Sheeler, Angelique Dains, Mary E. Kukla, Paul B. McCray, Jr, Stanley Perlman, Bradley Ford, Daniel J. Diekema, Melanie Wellington, Alejandro A. Pezzulo, Jorge L. Salinas
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 42 / Issue 12 / December 2021
- Published online by Cambridge University Press:
- 24 June 2021, pp. 1514-1516
- Print publication:
- December 2021
-
- Article
- Export citation
Informed consent: Old and new challenges in the context of the COVID-19 pandemic
- Erin Rothwell, Donna Brassil, Marietta Barton-Baxter, Kimberly A. Brownley, Neal W. Dickert, Daniel E. Ford, Stephanie A. Kraft, Jennifer B. McCormick, Benjamin S. Wilfond
-
- Journal:
- Journal of Clinical and Translational Science / Volume 5 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 07 April 2021, e105
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
In this paper, we address how the COVID-19 pandemic has impacted informed consent for clinical research through examining experiences within Clinical and Translation Science Award (CTSA) institutions. We begin with a brief overview of informed consent and the challenges that existed prior to COVID-19. Then, we discuss how informed consent processes were modified or changed to address the pandemic, consider what lessons were learned, and present research and policy steps to prepare for future research and public health crises. The experiences and challenges for CTSA institutions offer an important perspective for examining what we have learned about informed consent and determining the next steps for improving the consent process.
Personalized Intervention Program: Tobacco Treatment for Patients at Risk for Lung Cancer
- Krysten W. Bold, Benjamin A. Toll, Brenda Cartmel, Bennie B. Ford, Alana M. Rojewski, Ralitza Gueorguieva, Stephanie S. O'Malley, Lisa M. Fucito
-
- Journal:
- Journal of Smoking Cessation / Volume 13 / Issue 4 / December 2018
- Published online by Cambridge University Press:
- 11 December 2017, pp. 244-247
- Print publication:
- December 2018
-
- Article
- Export citation
-
Background: Lung cancer screening and tobacco treatment for patients at high-risk for lung cancer may greatly reduce mortality from smoking, and there is an urgent need to improve smoking cessation therapies for this population.
Aims: The purpose of this study is to test the efficacy of two separate, sequential interventions to promote tobacco cessation/reduction compared to standard care in smokers considered high-risk for lung cancer.
Methods: The study will recruit 276 current smokers attending a lung cancer screening clinic or considered high-risk for lung cancer based on age and smoking history across two sites. Patients first will be randomized to either standard tobacco treatment (8 weeks of nicotine patch and five individual counselling sessions) or standard tobacco treatment plus personalized gain-framed messaging. At the 8-week visit, all patients will be re-randomized to receive biomarker feedback or no biomarker feedback. Repeated assessments during treatment will be used to evaluate changes in novel biomarkers: skin carotenoids, lung function, and plasma bilirubin that will be used for biomarker feedback. We hypothesize that personalized gain-framed messages and receiving biomarker feedback related to tobacco cessation/reduction will improve quit rates and prevent relapse compared to standard care. Primary outcomes include 7-day point-prevalence abstinence verified with expired carbon monoxide at 8 weeks and mean cigarettes per day in the past week at 6 months.
Conclusions: Study findings will inform the development of novel interventions for patients at risk for lung cancer to improve smoking cessation rates.
Molecular Consequences of Cardiac Valve Development as a Result of Altered Hemodynamics
- Vinal Menon, Lorain Junor, John Eberth, Stephanie Ford, Matt McPheeters, Michael Jenkins, Marwa Belhaj, Jay Potts
-
- Journal:
- Microscopy and Microanalysis / Volume 23 / Issue S1 / July 2017
- Published online by Cambridge University Press:
- 04 August 2017, pp. 1330-1331
- Print publication:
- July 2017
-
- Article
-
- You have access Access
- Export citation
Bifidobacterium bifidum R0071 results in a greater proportion of healthy days and a lower percentage of academically stressed students reporting a day of cold/flu: a randomised, double-blind, placebo-controlled study
- Bobbi Langkamp-Henken, Cassie C. Rowe, Amanda L. Ford, Mary C. Christman, Carmelo Nieves, Jr, Lauren Khouri, Gretchen J. Specht, Stephanie-Anne Girard, Samuel J. Spaiser, Wendy J. Dahl
-
- Journal:
- British Journal of Nutrition / Volume 113 / Issue 3 / 14 February 2015
- Published online by Cambridge University Press:
- 21 January 2015, pp. 426-434
- Print publication:
- 14 February 2015
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Acute psychological stress is positively associated with a cold/flu. The present randomised, double-blind, placebo-controlled study examined the effect of three potentially probiotic bacteria on the proportion of healthy days over a 6-week period in academically stressed undergraduate students (n 581) who received Lactobacillus helveticus R0052, Bifidobacterium longum ssp. infantis R0033, Bifidobacterium bifidum R0071 or placebo. On each day, participants recorded the intensity (scale: 0 = not experiencing to 3 = very intense) for nine cold/flu symptoms, and a sum of symptom intensity >6 was designated as a day of cold/flu. B. bifidum resulted in a greater proportion of healthy days than placebo (P≤ 0·05). The percentage of participants reporting ≥ 1 d of cold/flu during the 6-week intervention period was significantly lower with B. bifidum than with placebo (P< 0·05). There were no effects of B. infantis or L. helveticus compared with placebo on either outcome. A predictive model accounted for influential characteristics and their interactions on daily reporting of cold/flu episodes. The proportion of participants reporting a cold on any given day was lower at weeks 2 and 3 with B. bifidum and B. infantis than with placebo for the average level of stress and the most commonly reported number of hours of sleep. Daily intake of bifidobacteria provides benefit related to cold/flu outcomes during acute stress.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Contributors
-
- By Nicholas B. Allen, Stephanie Assuras, Robert M. Bilder, Joan C. Borod, John L. Bradshaw, Warrick J. Brewer, Ariel Brown, Nik Brown, Tyrone Cannon, Audrey Carstensen, Cameron S. Carter, Luke Clark, Phyllis Chua, Thilo Deckersbach, Richard A. Depue, Tali Ditman, Aleksey Dumer, David E. Fleck, Lara Foland-Ross, Judith M. Ford, Nelson Freimer, Paolo Fusar-Poli, Nathan A. Gates, Terry E. Goldberg, George Graham, Igor Grant, Melissa J. Green, Michelle M. Halfacre, Wendy Heller, John D. Herrington, Garry D. Honey, Jennifer E. Iudicello, Henry J. Jackson, J. David Jentsch, Donald Kalar, Paul Keedwell, Ester Klimkeit, Nancy S. Koven, Donna A. Kreher, Gina R. Kuperberg, Edythe London, Dan I. Lubman, Daniel H. Mathalon, Patrick D. McGorry, Philip McGuire, George R. Mangun, Gregory A. Miller, Albert Newen, Jack B. Nitschke, Jaak Panksepp, Christos Pantelis, Mary Philips, Russell A. Poldrack, Scott L. Rauch, Susan M. Ravizza, Steven Paul Reise, Nicole Rinehart, Angela Rizk-Jackson, Trevor W. Robbins, Tamara A. Russell, Fred W. Sabb, Cary R. Savage, Kimberley R. Savage, J. Cobb Scott, Marc L. Seal, Larry J. Seidman, Paula K. Shear, Marisa M. Silveri, Nadia Solowij, Laura Southgate, G. Lynn Stephens, D. Stott Parker, Stephen M. Strakowski, Simon A. Surguladze, Kate Tchanturia, René Testa, Janet Treasure, Eve M. Valera, Kai Vogeley, Anthony P. Weiss, Sarah Whittle, Stephen J. Wood, Steven Paul Woods, Murat Yücel, Deborah A. Yurgelun-Todd
- Edited by Stephen J. Wood, University of Melbourne, Nicholas B. Allen, University of Melbourne, Christos Pantelis, University of Melbourne
-
- Book:
- The Neuropsychology of Mental Illness
- Published online:
- 10 May 2010
- Print publication:
- 01 October 2009, pp xv-xx
-
- Chapter
- Export citation






